Dialysis is a life-saving medical treatment used when the kidneys are no longer able to perform their essential functions. Healthy kidneys filter waste products, toxins, and excess fluids from the blood. When kidney function declines significantly due to chronic disease or injury, dialysis helps perform these critical tasks artificially.
In the United States, millions of people live with kidney disease, and many depend on dialysis to survive. According to the National Kidney Foundation, dialysis is a crucial treatment for individuals experiencing kidney failure, also known as end-stage renal disease (ESRD).

This guide explains what dialysis is, how it works, the different types of dialysis, and what patients in the United States should know about this essential treatment.
What Do the Kidneys Do?
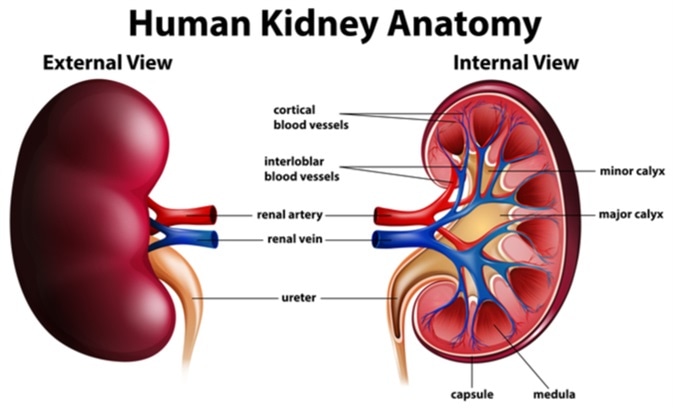
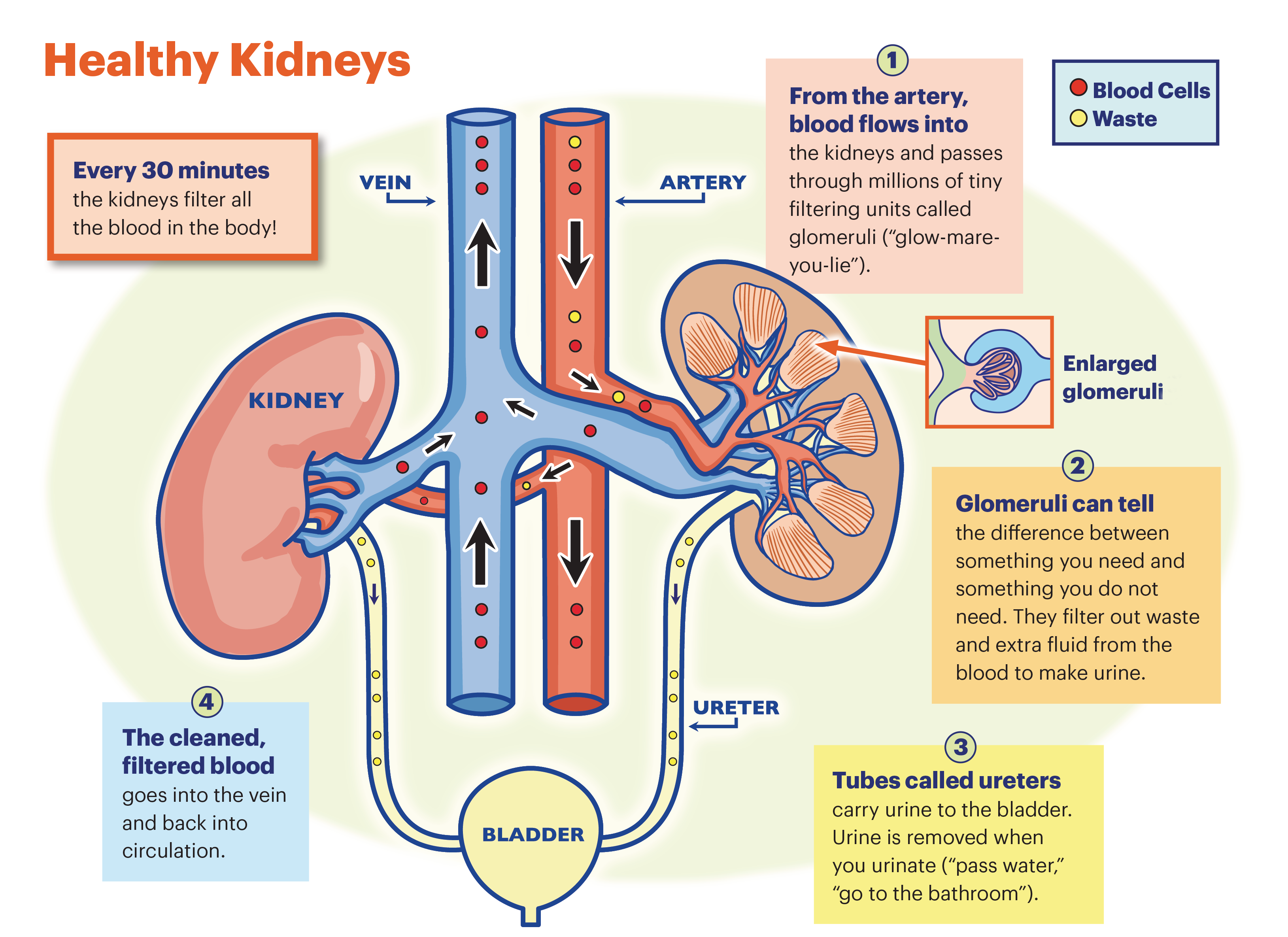
The kidneys are two bean-shaped organs located on either side of the spine, just below the rib cage. These organs play a vital role in maintaining the body’s internal balance.
Key functions of the kidneys include:
- Filtering waste products from the blood
- Removing excess fluid through urine
- Balancing electrolytes such as sodium and potassium
- Regulating blood pressure
- Producing hormones that support red blood cell production
When kidney function drops to about 10–15% of normal capacity, dialysis or a kidney transplant may become necessary.
What Is Dialysis?

Dialysis is a medical procedure that removes waste, toxins, and excess fluid from the blood when the kidneys can no longer perform these functions effectively.
The treatment works by:
- Filtering harmful substances from the bloodstream
- Maintaining proper electrolyte balance
- Removing extra fluids from the body
Dialysis does not cure kidney disease, but it helps patients maintain health and quality of life while managing kidney failure.
Healthcare organizations such as the Centers for Disease Control and Prevention emphasize that early detection and management of kidney disease can delay the need for dialysis.
Types of Dialysis
There are two main types of dialysis used in the United States: hemodialysis and peritoneal dialysis.
1. Hemodialysis

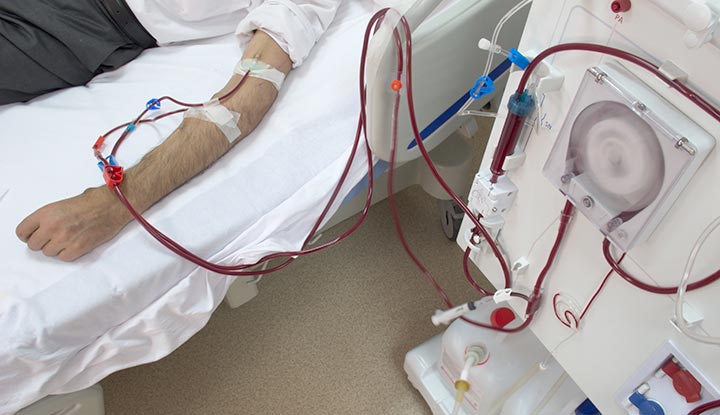
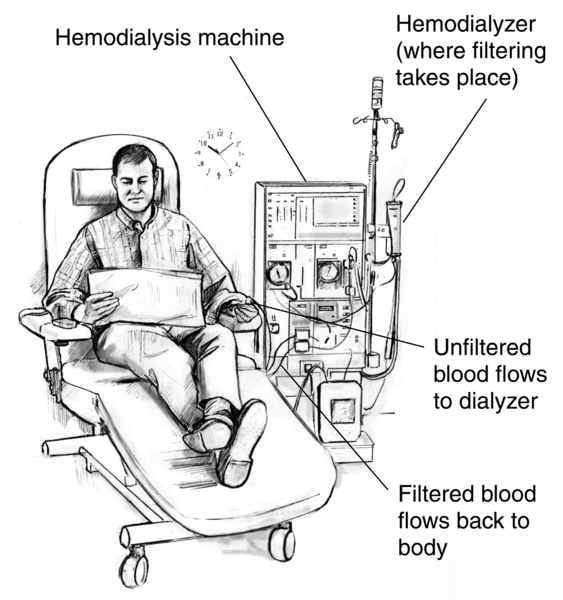
Hemodialysis is the most common form of dialysis. In this procedure, a machine filters the blood outside the body.
How Hemodialysis Works
- Blood is removed from the body through a vascular access point.
- The blood flows through a dialysis machine that filters waste products.
- The cleaned blood is returned to the body.
Treatment Schedule
Most hemodialysis patients receive treatment:
- Three times per week
- Each session lasting about 3–5 hours
Hemodialysis is typically performed at specialized dialysis centers or hospitals.
2. Peritoneal Dialysis

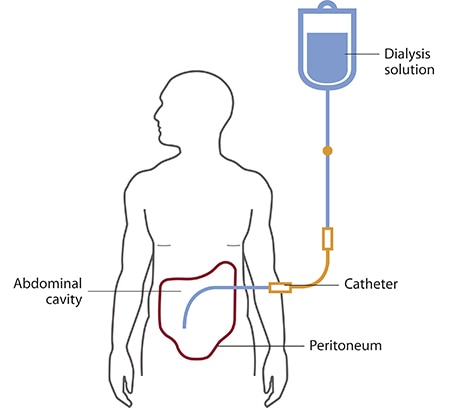
Peritoneal dialysis uses the lining of the abdomen (called the peritoneum) as a natural filter.
How Peritoneal Dialysis Works
- A dialysis fluid is placed into the abdomen through a catheter.
- Waste products and excess fluids pass from the blood into the dialysis fluid.
- The fluid is later drained and replaced with fresh solution.
Advantages of Peritoneal Dialysis
- Can often be performed at home
- Offers more flexible treatment schedules
- Allows greater independence for some patients
Doctors determine the most suitable type of dialysis based on the patient’s health condition and lifestyle.
Why Do People Need Dialysis?
Dialysis becomes necessary when kidneys fail to remove waste effectively. This condition is called kidney failure or end-stage renal disease (ESRD).
Common causes include:
Chronic Kidney Disease
Long-term kidney damage gradually reduces kidney function over time.
Diabetes
Diabetes is the leading cause of kidney failure in the United States.
High Blood Pressure
Uncontrolled hypertension can damage blood vessels in the kidneys.
Genetic Conditions
Inherited disorders such as polycystic kidney disease may affect kidney function.
Acute Kidney Injury
Sudden kidney failure caused by infection, injury, or medication toxicity may require temporary dialysis.
Signs That Dialysis May Be Needed

Symptoms of advanced kidney failure may include:
- Severe fatigue
- Swelling in the legs or ankles
- Shortness of breath
- Nausea and vomiting
- Difficulty concentrating
- Reduced urine output
Doctors use blood tests, urine tests, and imaging studies to determine when dialysis is necessary.
Life on Dialysis: What Patients Should Expect
Living with dialysis requires adjustments, but many people continue to lead productive and active lives.
Important lifestyle considerations include:
Dietary Adjustments
Patients often need to monitor their intake of:
- Sodium
- Potassium
- Phosphorus
- Fluids
Regular Medical Monitoring
Frequent checkups help ensure dialysis treatments are working effectively.
Emotional Support
Managing kidney disease can be challenging. Support from family, healthcare providers, and patient communities is essential.
Can Dialysis Be Avoided?
In some cases, early management of kidney disease may delay or prevent the need for dialysis.
Preventive strategies include:
- Managing blood pressure
- Controlling diabetes
- Eating a kidney-friendly diet
- Staying physically active
- Avoiding excessive use of certain medications
Regular health checkups help detect kidney problems early.
Kidney Transplant as an Alternative
For some patients, a kidney transplant may be an alternative to long-term dialysis.
A transplant replaces the failed kidney with a healthy donor kidney, potentially restoring normal kidney function.
However, not all patients are eligible for transplantation, and waiting lists for donor kidneys can be long.
Dialysis is a vital treatment that helps people with kidney failure live longer and maintain their health. By filtering waste and balancing fluids, dialysis performs the essential functions that damaged kidneys can no longer handle.
Understanding how dialysis works, recognizing the symptoms of kidney disease, and seeking early medical care can make a significant difference in managing kidney health.
For many Americans living with kidney disease, dialysis provides an opportunity to maintain quality of life while receiving the medical care they need.

